Children with autism, ADHD, sensory processing disorders, and other special needs face unique challenges in the dental chair that go far beyond typical childhood anxiety. According to the American Academy of Pediatric Dentistry’s 2024 guidelines, approximately 15% of children have special healthcare needs that can significantly impact their ability to receive routine dental care. As pediatric dentistry increasingly recognizes that traditional behavior management techniques often fall short for these young patients, sedation has emerged as a critical tool for ensuring both safety and successful treatment outcomes.
For families in Morgan Hill navigating these challenges, understanding how sedation works specifically for children with special needs can transform what might otherwise be traumatic dental experiences into manageable, even positive encounters. The stakes extend beyond just completing a single procedure — children who have negative early dental experiences often develop lasting dental phobias that persist into adulthood, creating lifelong oral health complications.
This comprehensive guide explores how different types of sedation support children with special dental needs, the safety protocols that make these procedures possible, and what parents can expect throughout the entire process.
How Sedation Supports Children With Special Dental Needs
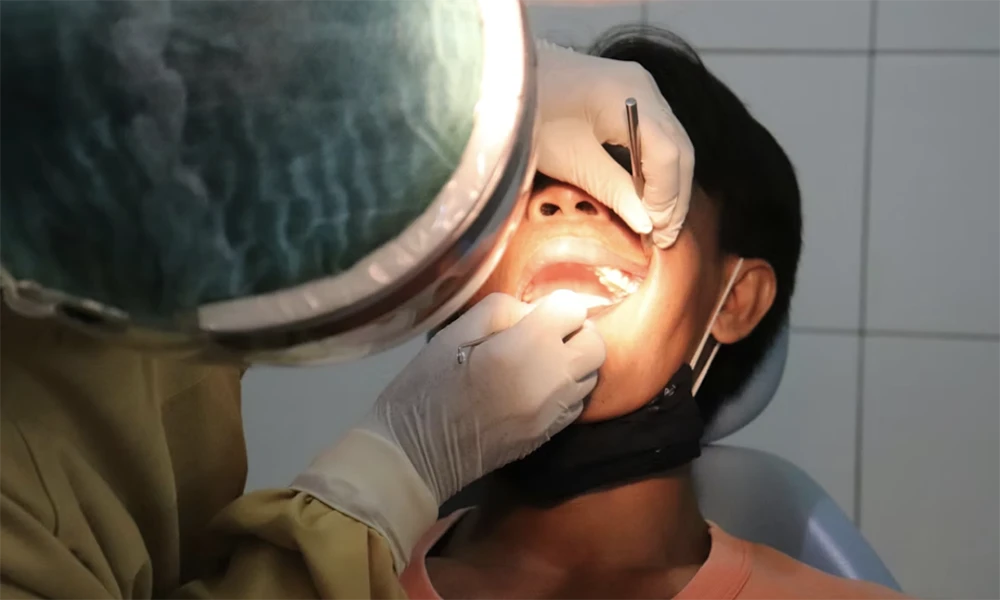
Children with special needs often experience heightened sensory sensitivities, difficulty processing instructions, or challenges remaining still for extended periods — all of which make standard dental procedures particularly difficult. The bright lights, unfamiliar sounds of dental equipment, and physical sensations of dental work can trigger overwhelming responses that traditional behavior management techniques simply can’t address effectively.
Sedation creates a buffer between these sensory challenges and the child’s ability to tolerate necessary dental care. Rather than forcing cooperation through restraint or repeated attempts that increase anxiety, sedation allows the child’s nervous system to remain calm while still maintaining essential reflexes and breathing functions. This approach proves especially valuable for children with autism spectrum disorders, who may have rigid behavioral patterns or extreme sensitivity to environmental changes.
The therapeutic benefits extend beyond just completing procedures. Children who receive appropriately administered sedation often have reduced anticipatory anxiety about future dental visits. For a child with developmental delays who might not understand why they need dental work, sedation eliminates the need for complex explanations and allows the dentist to work efficiently while the child remains comfortable.
Consider a seven-year-old with severe ADHD who needs multiple fillings — without sedation, the constant need to redirect attention and manage movement can turn a one-hour appointment into multiple stressful sessions. With appropriate sedation, the same work can be completed safely in a single visit, reducing overall stress for both the child and family while ensuring optimal treatment outcomes.
Types of Pediatric Dental Sedation Used in Morgan Hill
Pediatric sedation differs significantly from adult approaches, requiring specialized training and equipment designed specifically for children’s unique physiological needs. The choice of sedation method depends on the child’s specific condition, the complexity of required procedures, and individual medical history.
Nitrous Oxide and Oral Conscious Sedation
Nitrous oxide, commonly called “laughing gas,” represents the mildest form of sedation and often serves as the first-line approach for children with special needs who experience moderate anxiety or sensory sensitivities. The gas creates a relaxed, euphoric feeling while allowing children to remain fully conscious and responsive to instructions. For children with autism or sensory processing disorders, nitrous oxide can help reduce the overwhelming nature of dental stimuli without completely altering their awareness.
Oral conscious sedation involves liquid medications given by mouth, typically 30-60 minutes before treatment. This approach works particularly well for children who can’t tolerate the nasal mask required for nitrous oxide or need deeper relaxation for longer procedures. The medication creates a drowsy, calm state while preserving the child’s ability to respond to verbal commands and maintain protective reflexes.
The key advantage of these lighter sedation methods lies in their reversibility and minimal impact on the child’s respiratory function. Many children with developmental disabilities have underlying medical conditions that make deeper sedation riskier, making conscious sedation an ideal middle ground that provides comfort without excessive medical complexity.
General Anesthesia and IV Sedation in Pediatric Dentistry
For children with severe behavioral challenges or those requiring extensive dental work, deeper sedation options become necessary. General anesthesia renders the child completely unconscious, allowing dentists to perform complex procedures without any patient movement or distress. This approach often proves essential for children with profound developmental disabilities who cannot cooperate with dental care despite other interventions.
IV sedation provides a middle ground between conscious sedation and general anesthesia, creating deep relaxation while maintaining some level of consciousness. The medication can be adjusted throughout the procedure, giving the dentist precise control over the child’s sedation level. This flexibility makes IV sedation particularly valuable for procedures of uncertain duration or when a child’s response to lighter sedation proves inadequate.
Both options require hospital-grade monitoring and emergency equipment, along with dentists who have completed advanced sedation training. For families working with a kids sedation dentist in Morgan Hill, understanding these deeper sedation options helps set appropriate expectations for complex cases where lighter methods won’t suffice.
Safety Protocols and Risk Considerations in Pediatric Sedation
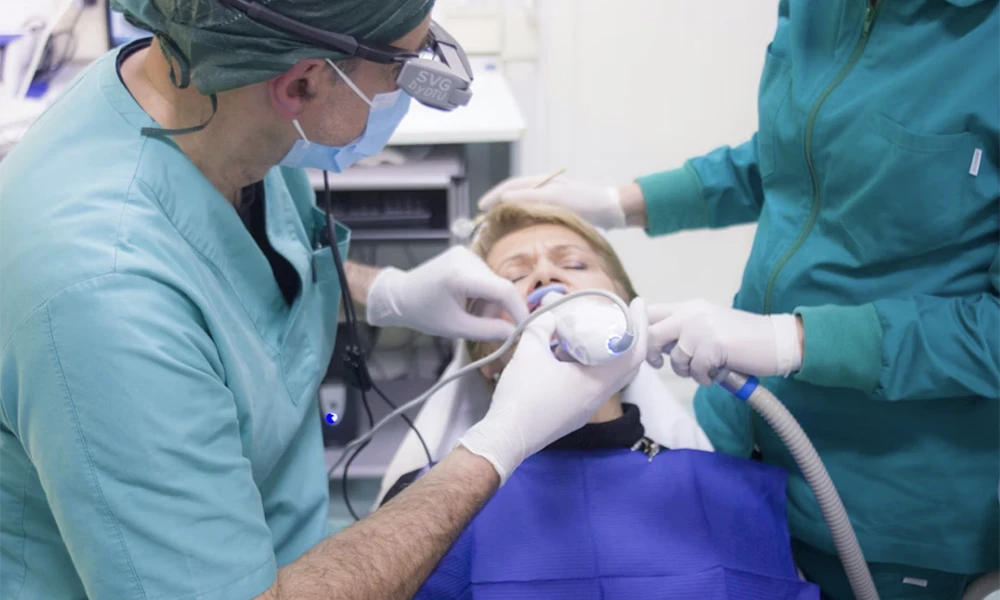
Modern pediatric sedation follows rigorous safety protocols developed specifically to address children’s unique physiological vulnerabilities. Children have different respiratory patterns, medication metabolism rates, and cardiovascular responses compared to adults, requiring specialized monitoring equipment and emergency procedures tailored to pediatric patients.
Pre-sedation medical evaluation serves as the foundation of safe pediatric sedation. This assessment reviews the child’s complete medical history, current medications, and any underlying conditions that might affect sedation response. Children with special needs often have complex medical histories including seizure disorders, cardiac conditions, or respiratory issues that require careful consideration when selecting sedation methods and dosing.
During the procedure, continuous monitoring tracks heart rate, blood pressure, oxygen saturation, and carbon dioxide levels. Modern pediatric sedation units include equipment sized appropriately for children, along with emergency medications calculated for pediatric dosing. The treating dentist maintains current certification in Pediatric Advanced Life Support (PALS), ensuring rapid response capability should any complications arise.
Risk-benefit analysis becomes particularly important for children with special needs because these patients often have the most to gain from successful sedation while potentially facing higher baseline medical risks. Research consistently shows that when appropriately administered by trained providers, pediatric dental sedation has an excellent safety record. The greater risk often lies in avoiding necessary dental care due to behavioral challenges, leading to dental infections or more complex procedures later.
Recovery monitoring continues until the child returns to baseline alertness and protective reflexes. For children with communication difficulties, staff trained in recognizing non-verbal signs of distress or complications provide specialized post-sedation care that accounts for each child’s individual needs.
Preparing Children and Parents for Dental Sedation
Successful sedation experiences begin long before the child enters the dental office, requiring thoughtful preparation that accounts for both the child’s special needs and the family’s anxiety levels.
Pre-Sedation Preparation Guidelines for Parents
Medical preparation starts with a comprehensive review of the child’s current health status, including any recent illnesses, medication changes, or behavioral patterns that might affect sedation response. Parents must follow specific fasting instructions — typically no solid food for 6-8 hours and clear liquids for 2-3 hours before sedation — though exact timing varies based on the child’s age and sedation method.
For children with autism or developmental delays, maintaining familiar routines becomes crucial. Parents should discuss any comfort objects, preferred communication methods, or behavioral triggers with the dental team beforehand. Some children benefit from social stories or visual schedules that help them understand the upcoming procedure, while others find such preparation overwhelming and do better with minimal advance discussion.
Medication management requires particular attention for children already taking psychiatric medications, seizure medications, or other drugs that might interact with sedation agents. The dental team coordinates with the child’s pediatrician to determine whether existing medications should be continued, adjusted, or temporarily discontinued before sedation.
Managing Anxiety and Comfort During Dental Visits
Environmental modifications can significantly impact a special needs child’s comfort level during sedation appointments. Many pediatric dental offices offer sensory-friendly appointment times with dimmed lighting, reduced noise levels, and minimal waiting room activity. Some facilities provide weighted blankets, noise-canceling headphones, or other comfort items that help children with sensory processing challenges remain calm.
Communication strategies must align with each child’s developmental level and preferred learning style. Children with autism often respond well to clear, concrete explanations using visual aids, while those with attention deficits benefit from simple, step-by-step instructions given immediately before each action. The dental team’s ability to read non-verbal cues becomes essential for children who cannot verbally express discomfort or confusion.
Parental presence policies vary depending on sedation type and individual circumstances. While parents can typically remain present during lighter sedation, deeper sedation often requires parental separation for safety reasons. Preparing both child and parent for these transitions helps prevent last-minute complications that could delay or cancel procedures.
Post-Sedation Care and Impact on Future Dental Visits
Recovery from pediatric sedation requires specialized monitoring that accounts for children’s unique physiological responses and communication abilities. Unlike adults who can clearly express how they feel, children may show confusion, irritability, or altered behavior patterns that require experienced interpretation.
The immediate recovery period focuses on ensuring stable vital signs and return of protective reflexes before discharge. Children with special needs may experience longer or more variable recovery times, particularly those with underlying neurological conditions or those taking medications that affect brain function. Staff monitor for adequate breathing, appropriate responsiveness, and ability to maintain head position independently.
Behavioral changes during recovery can be particularly pronounced in children with autism or developmental delays. Some children become unusually clingy or withdrawn, while others may exhibit temporary regression in communication or self-care skills. Parents receive detailed instructions about normal versus concerning post-sedation behaviors, along with clear guidelines about when to contact the dental office or seek emergency care.
Long-term outcomes show that appropriate use of sedation often improves children’s tolerance for future dental care. When children associate dental visits with comfort rather than distress, they’re more likely to cooperate with preventive care as they mature. This positive conditioning proves especially valuable for children with special needs who will require ongoing dental supervision throughout their lives.
The documented procedure notes become part of the child’s dental record, helping future providers understand what sedation methods worked well and any unique considerations for that individual patient. This continuity proves invaluable for children who may see multiple specialists or require care from different providers as they grow.
For families navigating the complex intersection of special needs and dental care, understanding that sedation represents a therapeutic tool rather than just a convenience can fundamentally shift expectations about their child’s long-term oral health outcomes. The goal extends beyond simply completing necessary procedures — it’s about establishing a foundation for lifelong dental wellness that acknowledges and accommodates each child’s unique needs.





