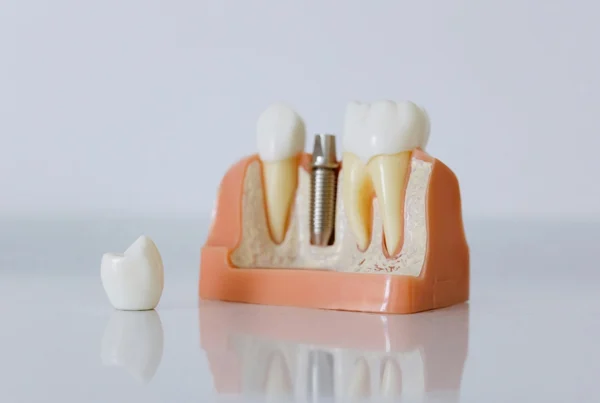
The American Dental Association reports that over 36 million Americans have no teeth, with millions more facing complete tooth loss within the next decade. As dental implant technology advances and success rates climb above 95%, full arch dental implants have emerged as the gold standard for complete mouth restoration — yet many people still wonder whether they qualify for this life-changing treatment.
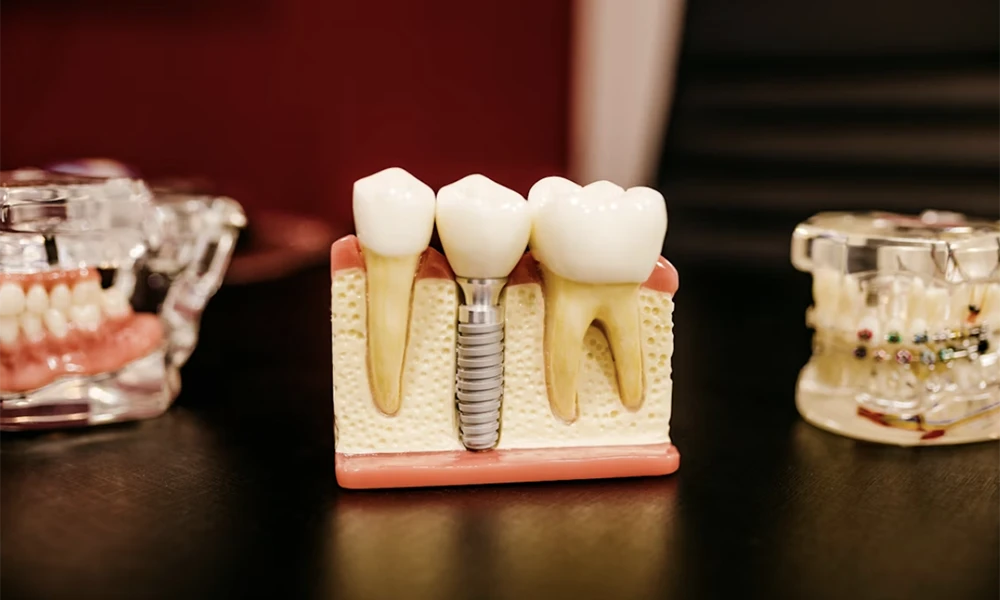
The shift away from traditional dentures reflects a growing understanding of how tooth loss affects more than just eating and speaking. When you lose all your teeth, your jawbone begins deteriorating immediately, changing your facial structure and accelerating aging. Full arch implants don’t just replace missing teeth — they preserve the bone that supports your facial features and restore bite force to near-natural levels.
For anyone considering this investment in their oral health, understanding candidacy involves more than age or budget considerations. Your bone density, overall health, lifestyle factors, and realistic expectations all play crucial roles in determining whether full arch implants will deliver the transformative results you’re seeking. The evaluation process reveals not just whether you’re a candidate, but how to optimize your chances for decades of successful function.
How Full Arch Implants Improve Oral Health and Lifestyle
Full arch implants fundamentally change how your mouth functions compared to traditional dentures or no teeth at all. Unlike removable dentures that rest on your gums and can slip during eating or speaking, implants anchor directly into your jawbone, providing the stability needed for confident chewing and clear speech.
The bite force restoration is particularly dramatic. Natural teeth generate about 200-250 pounds of pressure per square inch when chewing, while conventional dentures typically provide only 50-60 pounds of force. Full arch implants restore roughly 80-90% of your original bite strength, allowing you to eat foods that denture wearers often have to avoid — fresh apples, nuts, corn on the cob, and chewy meats.
Speech improvements often surprise patients the most. Missing teeth and ill-fitting dentures create air gaps that affect pronunciation, particularly with “s” and “f” sounds. Full arch implants eliminate these gaps entirely, restoring natural speech patterns within weeks of the final restoration placement. Many patients report feeling more confident in social situations once they no longer worry about denture movement or whistling sounds.
Perhaps most importantly, implants preserve your facial bone structure. When teeth are missing, your jawbone begins resorbing within months, leading to the sunken facial appearance common in denture wearers. The titanium implants stimulate bone tissue through a process called osseointegration, maintaining bone density and preventing the facial collapse that ages denture wearers prematurely. This bone preservation effect continues working for decades, making implants an investment in your long-term facial aesthetics as well as oral function.
What to Expect During the Full Arch Implant Procedure
The full arch implant process typically unfolds in carefully planned phases, though modern techniques increasingly allow for immediate placement of temporary teeth on the same day as implant surgery. Your treatment begins with comprehensive imaging — usually 3D CT scans — that allow your periodontist to map your jawbone density and plan precise implant placement before surgery begins.
On surgery day, you’ll receive sedation appropriate for your comfort level, ranging from local anesthesia to IV sedation. The procedure itself involves placing four to six implants per arch, strategically angled to maximize contact with available bone. Many patients are surprised that the discomfort is less than they anticipated — most report it feels similar to having several teeth extracted, with manageable pain controlled by prescription medication for just a few days.
The immediate post-surgery period requires careful attention to your diet and oral hygiene. You’ll likely receive temporary teeth attached to your new implants within 24-48 hours, allowing you to eat soft foods and maintain a normal appearance while healing progresses. These temporaries aren’t as strong as your final restoration, so you’ll need to stick with softer foods for several weeks.
Healing and Osseointegration Process
The critical healing phase spans three to six months, during which your jawbone grows around and fuses with the titanium implants. This biological process, called osseointegration, creates the foundation for your implants’ long-term stability. During this period, blood vessels and bone cells colonize the implant surface, essentially making the titanium posts part of your jaw structure.
Most patients find this healing period more comfortable than expected. While you’ll need to avoid hard foods and maintain excellent oral hygiene, many people continue working and maintaining their normal routines within days of surgery. The temporary teeth allow you to eat most soft foods and speak clearly, so the social disruption is minimal compared to the months of adjustment often required with new dentures.
Role of Bone Grafting and Preparation
About 60% of full arch implant candidates require some degree of bone grafting to ensure adequate implant support. Bone loss from long-term tooth absence, gum disease, or previous extractions often leaves insufficient bone height or width for optimal implant placement. Modern grafting techniques can rebuild these areas using synthetic materials, processed donor bone, or your own bone harvested from other sites.
The grafting process might extend your treatment timeline by three to six months, but it significantly improves your long-term success odds. Areas that receive grafting before implant placement show success rates comparable to sites with natural bone density. Your periodontist will determine during the planning phase whether grafting is necessary and can often combine it with implant placement to minimize the number of surgical procedures required.
Who Qualifies as a Good Candidate for Full Arch Implants?
Successful full arch implant candidates share several key characteristics, though age alone rarely disqualifies someone from treatment. The most critical factor is having adequate bone density to support the implants, which can often be addressed through bone grafting if natural bone is insufficient. Good candidates also demonstrate commitment to excellent oral hygiene and have realistic expectations about the treatment process and outcomes.
Your overall health status plays a significant role in candidacy evaluation. Uncontrolled diabetes, active cancer treatment, heavy smoking, and certain medications can interfere with healing and osseointegration. However, many medical conditions that once excluded patients from implant treatment are now manageable with proper coordination between your dentist and physician. Even patients with controlled diabetes often achieve excellent implant success when their blood sugar levels remain stable.
Lifestyle factors matter more than many people realize. Successful implant patients typically commit to twice-daily brushing, daily flossing, and regular professional cleanings. They also understand that while implants don’t get cavities, the gums and bone around them require ongoing care to prevent peri-implantitis — a condition similar to gum disease that can threaten implant stability.
Financial commitment extends beyond the initial treatment cost. Quality full mouth dental implants require ongoing maintenance, including professional cleanings every three to four months and potential repairs or adjustments over time. Candidates who view implants as a long-term investment rather than a one-time expense tend to experience better outcomes and higher satisfaction.
Candidacy Criteria for Seniors
Age itself doesn’t disqualify someone from full arch implants — in fact, many of the most satisfied patients are in their 70s and 80s. Older adults often have more time to dedicate to proper healing and maintenance, and they frequently experience the most dramatic quality-of-life improvements since they may have struggled with denture problems for years.
Senior candidates do require more careful health evaluation, particularly regarding medications that affect healing. Blood thinners, bisphosphonates for osteoporosis, and certain heart medications may require coordination with your physician to modify dosing around surgery. However, these medical considerations rarely prevent treatment — they simply require additional planning and monitoring.
The bone density concerns common in older adults, particularly post-menopausal women, can usually be addressed through grafting techniques. Many seniors actually prove to be ideal candidates because they’re motivated to invest in their long-term comfort and are often past the child-rearing years when time and financial resources might be limited.
Health Conditions That May Impact Candidacy
Several medical conditions require special consideration but don’t automatically disqualify you from implant treatment. Diabetes patients with HbA1c levels below 7% typically heal successfully, though they may need longer healing periods and more frequent monitoring. Your endocrinologist and periodontist will work together to optimize your blood sugar control before and after surgery.
Osteoporosis and medications used to treat it present more complex considerations. Bisphosphonates like Fosamax can interfere with bone healing, but the risk varies significantly based on how long you’ve taken the medication and whether it’s oral or IV administered. Many patients can safely receive implants with medication modifications and extended healing periods.
Smoking remains the most significant modifiable risk factor for implant failure. Nicotine restricts blood flow to healing tissues and dramatically increases infection risk. While some practitioners require complete smoking cessation, others work with patients to minimize tobacco use before and after surgery, recognizing that perfect is often the enemy of good in improving someone’s quality of life.
Long-Term Success, Care, and Risks of Full Arch Implants
Full arch implants demonstrate impressive longevity when properly maintained, with studies showing 95-98% success rates at 10 years and many implants functioning well beyond 20 years. These success rates exceed those of other tooth replacement options by significant margins, making implants a sound investment for most candidates despite their higher upfront cost.
The key to long-term success lies in understanding that while implant crowns can’t get cavities, the supporting tissues require vigilant care. Peri-implantitis, an inflammatory condition affecting the gums and bone around implants, poses the greatest threat to implant longevity. This condition develops similarly to gum disease but progresses more rapidly around implants than natural teeth, making prevention through excellent hygiene and regular professional care essential.
Daily maintenance involves more than standard brushing and flossing. Most successful implant patients use water flossers or specialized implant brushes to clean around the implant posts, and many benefit from antimicrobial mouth rinses. Professional cleanings typically occur every three to four months rather than the standard six-month intervals, allowing your dental team to monitor the implant sites closely and address any early signs of inflammation.
Realistic expectations help prevent disappointment and ensure long-term satisfaction. While implants restore most of your original chewing ability, they won’t feel exactly like natural teeth, particularly during the first year as you adapt to the new sensations. The adjustment period involves learning to chew differently and becoming accustomed to the way food feels against your new teeth. Most patients adapt completely within six to twelve months, often reporting they forget they have implants at all.
Common misconceptions about implant risks often deter good candidates from pursuing treatment. While complications can occur, serious problems like nerve damage or sinus injuries are rare when treatment is performed by experienced specialists using modern imaging and surgical techniques. The most common complications involve minor infections or temporary numbness that resolve with appropriate treatment.
How Do Full Arch Implants Compare to Traditional Dentures?
The functional differences between full arch implants and traditional dentures are substantial enough that many patients describe the experience as life-changing. Dentures rely on adhesive and suction for retention, which inevitably fails during eating or speaking. Even well-fitted dentures slip periodically, creating social anxiety and limiting food choices to softer options that won’t dislodge the appliance.
Full arch implants eliminate retention concerns entirely. The mechanical connection between implant and crown means your teeth can’t shift, slip, or fall out regardless of what you’re eating or how vigorously you’re chewing. This stability allows you to bite into foods with confidence and speak without worrying about denture movement creating embarrassing sounds or speech impediments.
The comfort differences extend beyond stability. Traditional dentures cover your palate and gums, dulling taste sensation and creating a bulky feeling that many wearers never fully accept. Implant-supported crowns expose your palate and require no coverage of healthy gum tissue, preserving normal taste and oral sensation. Many patients report that food tastes better and feels more natural after receiving implants.
Bone preservation represents perhaps the most significant long-term advantage of implants over dentures. Dentures actually accelerate bone loss by placing pressure on the gum ridges during chewing, gradually destroying the very tissues they depend on for support. This creates a cycle where dentures fit progressively worse over time, requiring frequent adjustments, relines, and eventual replacement. Full arch implants stimulate bone preservation through osseointegration, maintaining your facial structure and ensuring consistent fit for decades.
The maintenance requirements differ substantially as well. Dentures require daily removal for cleaning, overnight soaking, and regular application of adhesives. They need professional relines every few years and complete replacement every 5-10 years as your bone structure changes. Implants require the same daily brushing and flossing as natural teeth, with no removal necessary and no adhesives required. While the initial investment is higher, the long-term maintenance costs often favor implants when calculated over decades of use.
Your choice between these options ultimately depends on your priorities, health status, and willingness to invest in long-term oral health. For candidates who qualify medically and financially, the evidence strongly supports implants as the superior option for function, comfort, and bone preservation. However, dentures remain a viable solution for patients who cannot undergo surgery or prefer a less invasive approach to tooth replacement.
The decision becomes clearer when you consider the trajectory of each treatment over time. Denture wearers often find their quality of life gradually declining as bone loss progresses and appliance fit deteriorates, while implant patients typically experience stable or improving function as they adapt to their new teeth. This difference in long-term outlook makes the candidacy evaluation process crucial for determining which path will serve your needs best in the years ahead.